
OR
More from Author
National regulatory bodies in medical and nursing education should put their efforts together in integrating simulation with the current conventional education models
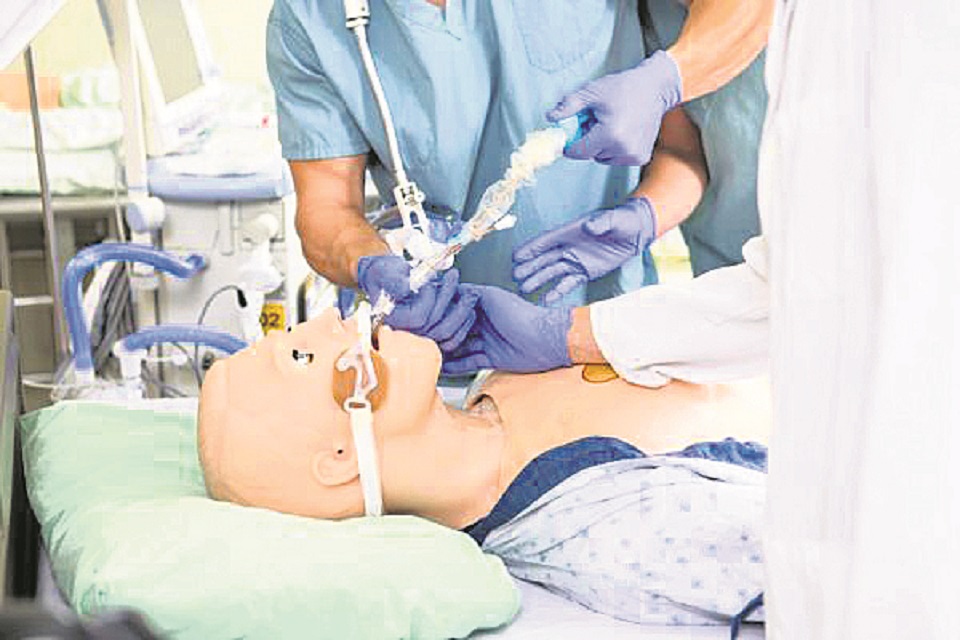
I still remember my internship days in 2009 at Mayo Hospital: a 2400-bed hospital with high bad occupancy in Lahore, Pakistan. I visualize my senior teaching me intubation in the emergency room, saying “the patient is deteriorating, put in the laryngoscope, visualize vocal cords and intubate quickly.” Unfortunately, my first attempt at intubation on the patient failed and my senior had to reintubate the patient.
I have a distinct memory of doing a per vaginal examination in pregnant mother and never being able to figure out the findings, as per vaginal examination was such a blind procedure! Trying to learn in a real patient was embarrassing for me as a young medical student and for the young mother-to-be! But, that was the best chance that I had.
During my internship, almost on every Friday, we saw gunshot injuries and mass casualties with multiple fractures/injuries in our emergency room. I, as an intern, was not competent in managing such crisis at all—neither clinically, nor emotionally. There was no training of trauma management that we received as young medical students.
After graduating from medical school and having worked few years as a medical officer, I realized that clinical medicine was not my cup of tea. I chose public health instead so that I could contribute to disease prevention rather than catering to the diseased patients.
In 2014, I was one of the few national trainers in one of the national skill labs in New Delhi, India. As a trainer, this was a new experience for me, as I was never aware that training/teaching could be done using models/manikins instead of real patients. Most of the skills of maternal and newborn health including per-vaginal examination were taught in the skills lab and the participants could practice again and again till they were competent and confident in doing it. Such a safe environment to learn and practice! I would imagine what if I had been trained like this as a medical student. How confident I would be as a student, as I taught various skills to participants until they got competent at it in the skills lab. I only wished…
In 2017, after joining Laerdal, I was trained in Simulation Based Education methodology. With the Stavanger Acute Medicine Foundation for Education and Research (SAFER) team, from Norway, in one of the EU-Sim courses we ran a scenario on Crisis Resource Management “how do you mange when you have multiple patients together” I vividly remembered my Fridays as an intern during the scenario.
I realized how important it is to learn the non-technical skills like communication, team work, leadership when it comes to managing any clinical case, even more so a CRISIS. Simulation is not only about learning technical skills, but a variety of human factors that affect the patient outcome.
In December 2019, I was at the Stavanger Acute Medicine Foundation for Education and Research (SAFER) in Norway and the faculty ran a simulation scenario on Medical Ethics. The session was an eye opener for me. It was a scenario of a cancer patient at a terminal stage, tired of going to the hospital and wanted to die at home. In his care, the wife had not been able to sleep many nights and thus wanted to send him to the hospital. She calls the nurse at home but the husband tells the nurse that he does not want to go. The nurse was in an ethical dilemma.
I had never even imagined that a topic like ethics could be taught in such a way. Ethics, although very important subject, was one of the most boring and uninteresting for us during medical school. The more I run simulations, the more I understand its value and the more I love it. Sky is the limit for learning through simulation.
At present, my efforts are dedicated to establish simulation based healthcare education in Nepal. In partnership with Laerdal and GIZ, in 2019, the first Simulation Lab in the country was established in Dhulikhel Hospital. Several midwives, nurses and medical doctors in the country have been trained since. The first EU Simulation Instructor Course was conducted in Nepal in 2020. We have also established the Simulation Society of Nepal and I am its current President. The Society is working in partnership with UNICEF Nepal to implement In-situ simulation based trainings in three hospitals in Province 2. A national manual on simulation based education is also being developed in partnership with the Ministry of Health and Population. This is just the beginning and there is so much more that needs to be done.
Every year, thousands of medical students graduate from various national and international institutions. I am sure their plight and mine, as a young medical doctor, resonate. After having learned so much about simulation and trained many, I highly encourage our national regulatory bodies in medical and nursing education to put their efforts together in integrating simulation with the current conventional education models. After all, well trained doctors and nurses are what the country needs and what the patients benefit most from.
The author, President of Simulation Society of Nepal, also represents Laerdal in Nepal
You May Like This
Doctors and development
Some doctors are not sympathetic to their patients. They launch their stethoscopes at private clinics and hospitals against their patients... Read More...

Tension rises in Dhulikhel hospital after the death of a patient
BANEPA, March 2: Dhulikhel Hospital has courted controversy after the death of a patient who was admitted there for the treatment... Read More...

Children’s hospital tense following death of a patient
KATHMANDU, Aug 23: The Basundhara-based Ishan Children and Women's Hospital in Kathmandu remained tensed on Tuesday, following vandalism by the... Read More...



Just In
- CM Kandel requests Finance Minister Pun to put Karnali province in priority in upcoming budget
- Australia reduces TR visa age limit and duration as it implements stricter regulations for foreign students
- Govt aims to surpass Rs 10 trillion GDP mark in next five years
- Govt appoints 77 Liaison Officers for mountain climbing management for spring season
- EC decides to permit public vehicles to operate freely on day of by-election
- Fugitive arrested after 26 years
- Indian Potash Ltd secures contract to bring 30,000 tons of urea within 107 days
- CAN adds four players to squad for T20 series against West Indies 'A'













Leave A Comment