
OR
Antimicrobial resistance amid Covid-19
Published On: December 20, 2020 07:00 AM NPT By: Sandeep Thapa


Sandeep Thapa
The author is Research Officer at Kathmandu Center for Genomics and Research Laboratory (KCGRL)news@myrepublica.com
Appropriate handling of future pandemics will require all actions to be focused on decreasing the spread and development of antimicrobial resistance.
Prolonged Covid-19 crisis has created unprecedented challenges in health and economy, further worsening the already precarious situation of Nepal’s most vulnerable health care system. Nepal is still in a critical period in its fight against the pandemic. Public health experts believe that infections are far more widespread than what official tallies show and that the numbers will rise if testing facilities are not enhanced.
Similarly, there has been a swelling burden of antimicrobial resistance (AMR) in the nation along with the prevalence of resistant superbugs. The resistance to antimicrobial agents by microorganisms causes AMR leading to its survival and replication. In humans, overuse and inappropriate usage of antibiotics, empirical antibiotic therapy, and irrational prescription of powerful antibiotics are substantial contributors to the growth of antibiotic resistance.
Much before Covid-19, the world had faced the threat of antimicrobial resistance. Many have sounded the alarm over further escalation during the pandemic. Furthermore, the practice of telecommunication with patients with mild symptoms has lessened the possibility of performing relevant clinical examinations and diagnostic tests.
Unpredictably, overuse of antibiotics would contribute to an increase in resistance against several classes of antibiotics. Prescription of effective antibiotics is crucial for the management of bacterial infections. However, antibiotics can’t be used against viral infections, of which Covid-19 is one.
During the current pandemic, studies have shown that half of the patients with Covid-19 have a bacterial co-infection. A report said that 71 percent of Covid-19 patients received antibiotics while only four percent had true bacterial co-infection.
Over the years, antibiotics have been foundational to healthcare systems and medical advancements across the world. However, due to wide-ranging causes, we are witnessing a continuous rise of resistance to antibiotics which is threatening the world with a catastrophic public health emergency in the years to come. Correspondingly, Covid-19 patients may develop secondary nosocomial infections with bacteria and fungi as a result of critical illness and prolonged hospitalizations. There is a concern that antimicrobials may be overused, followed by difficulty in diagnosing actual concurrent or secondary bacterial or fungal infections.
In this situation, Covid-19 might be causing a rise in the inappropriate use of antibiotics, mainly broad-spectrum antibiotics. Excessive and inappropriate use of broad-spectrum antibiotics is one of the main causes of the development of AMR. An increasing number of patients with undefined upper and lower respiratory tract symptoms, along with high fever, might be putting doctors under pressure to recommend antibiotics. Consequently, this pandemic encounters all aspects of healthcare encompassing both recognition and supervision of serious acute bacterial infection and effective delivery of antimicrobial stewardship. Serious bacterial infections may be missed when all attention will be focused on Covid-19.
It is, therefore, necessary to empirically treat the bacterial infection for those who are in home isolation.
The long fight to control the progress and spread of AMR is at a critical moment. The way we, as a global society, respond to the Covid-19 challenges now may affect our ability to fight AMR. In this scenario, the government should bring Antimicrobial stewardship programs (ASPs) to support hospitals’ Covid-19 response efforts. Potential ASP activities can include identifying patients with the disease, developing diagnostic and treatment protocols and disseminating these to providers, and optimizing guideline-concordant treatment.
Globally, there has been a proactive focus on dealing with such problems holistically with a ‘one-health’ approach. Several initiatives have been taken to bring different stakeholders from the ministries of health, environment, water, agriculture, and science and technology together to work on AMR.
Covid-19 will eventually disappear but AMR will not. The appropriate handling of future pandemics will require all actions to be focused on decreasing the spread and development of AMR.
The actual state of vulnerabilities or the risks in the community remain unknown. Thus it is essential to carefully scrutinize the parallels and interactions between Covid-19 and AMR. Collecting data to measure the impact of Covid-19 should be encouraged and authorities should bring programs focused on AMR. AMR testing of bacterial pathogens, establishing a laboratory networking, bringing External Quality Assessment (EQA) program, promoting standardized recording and reporting, routinely analyzing and disseminating data for advocacy and national policy adaptations should be the priorities.
Given the potential for significant antimicrobial use, antimicrobial stewardship activities should be implemented in monitoring antibiotic use to prevent the emergence of drug resistance during the pandemic.
Covid-19 pandemic provides an opportunity for ASPs to strengthen and enhance relationships with specialized groups within health systems. Covid-19 has galvanized the expansion of several well-facilitated laboratories in Nepal, and provided an opportunity to drive forward modernization in health sector. This opportunity should be used also to control the progress and spread of AMR.
The author is a research officer at Kathmandu Center for Genomics and Research Laboratory, Lalitpur
You May Like This
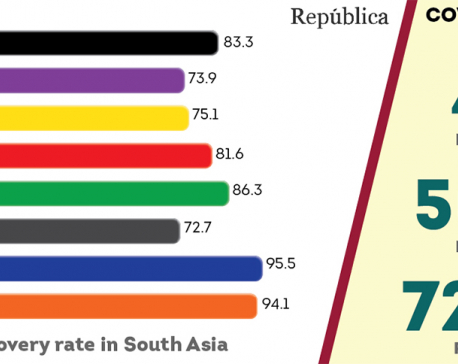
Nepal’s COVID-19 recovery rate is the lowest among SAARC countries
COVID-19 recovery tally goes past 50,000 ... Read More...

INFOGRAPHICS: These 52 districts are under lockdown
All eight districts in Province 2 are under lockdown amid worsening COVID-19 situation ... Read More...
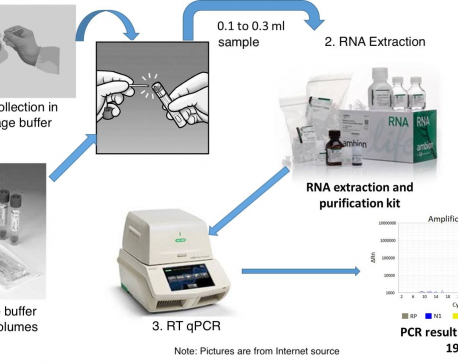
Can the new PCR kits purchased by the Army still be used? Yes!
Nepal has been under lockdown for more than three month now due to the ongoing pandemic of Covid-19. Nepal has... Read More...





Just In
- Challenges Confronting the New Coalition
- NRB introduces cautiously flexible measures to address ongoing slowdown in various economic sectors
- Forced Covid-19 cremations: is it too late for redemption?
- NRB to provide collateral-free loans to foreign employment seekers
- NEB to publish Grade 12 results next week
- Body handover begins; Relatives remain dissatisfied with insurance, compensation amount
- NC defers its plan to join Koshi govt
- NRB to review microfinance loan interest rate











Leave A Comment